Radiotherapy
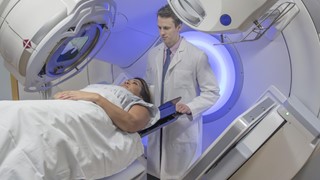
Radiotherapy is the treatment of cancer with ionising radiation, and can be used as the main form of treatment instead of surgery or in conjunction with the surgical removal of tumours by either decreasing tumour size before removal, or targeting any sections of tumour that may remain after surgery. It is also used in combination with chemotherapy in an attempt to maximise the effect on the tumour tissue.
There are various types of radiotherapy. Brachytherapy, where radioactive wires or seeds are implanted inside the body close to or directly within a tumour. Alternatively, in targetted radionuclide therapy a radioactive liquid that cancerous cells absorb is swallowed or injected. External beam therapy is the most commonly used technique and involves directing a beam of radiation in the form of X-rays, electrons or protons at a tumour from outside the body.
Who needs it?
Radiotherapy is a treatment for disease which is localised. Patients with cancerous tumours in organs or near body cavities, such as the prostate, may be treated with brachytherapy. Many other forms of cancer can be treated by external beam therapy. Some thyroid and blood disorders can also be treated.
How does it work? 
Radiotherapy uses the energy from radiation to kill cancerous cells. For brachytherapy treatments, commonly caesium-137 or iridium-192 are used and left in place for up to a few days. Alternatively sources emitting a particularly high dose of radiation are inserted for just a few minutes. Small sealed radioactive sources can also be permanently implanted. For example, iodine-125 seeds can be used to treat prostate cancer in its early stages.
In external beam radiotherapy, different radiation types and numbers of beams are used depending on the cancer requiring treatment. The therapy is usually delivered over a period of weeks, so that the total radiation dose is given in small fractions to keep unwanted side effects - that can range in severity from nausea to new cancers - to a minimum. These side effects occur because the energy from the radiation that kills the cancerous cells also damages the healthy tissue that it passes through. Treatment plans are designed to minimise the dose to the healthy tissues.
One way of doing this is to match the shape of the radiation beam to the tumour by using shielding materials to stop unwanted radiation. This also allows a greater dose to be used, increasing its effectiveness. Intensity Modulated Radiotherapy reduces such damage by using a combination of detailed imaging of the tumour prior to treatment and computer controlled delivery of the radiation beam so different radiation doses can be delivered to specific parts of the tumour.
Alternatively, using protons (positively charged particles) or positive ions (in this case, atoms that have had all their electrons removed) instead of X-rays or gamma rays reduces damage as instead of affecting all the tissue they pass through, most of their energy can be deposited directly within cancerous cells.
In all cases it is vital to know the position and shape of the tumour as accurately as possible to reduce radiation damage to healthy tissues. Both CT imaging (X-rays taken at many different angles through the body), and MRI can be used to determine this prior to radiotherapy treatment. The required dose and distribution of radiation within the patient must also be accurately calculated.
Future developments
Arc radiotherapy is gradually coming into use in the UK, and involves delivering radiation in one continuous arc round the patient while modifying the radiation field shape. 3-D imaging is being used to ensure treatment accuracy and to correct for organ movement and breathing.
Tomotherapy allows radiation to be delivered at all angles round a patient, in this case following precise analysis of the tumour shape via detailed imaging prior to delivery of every fraction of the treatment. Meanwhile stereotactic radiosurgery is increasingly being used to treat brain lesions, and involves the use of a high intensity radiation beam targeted so accurately that the entire radiation dose required for treatment can be given during a single procedure. This technique is now beginning to be applied to sites outside the head and is the subject of much development and research.